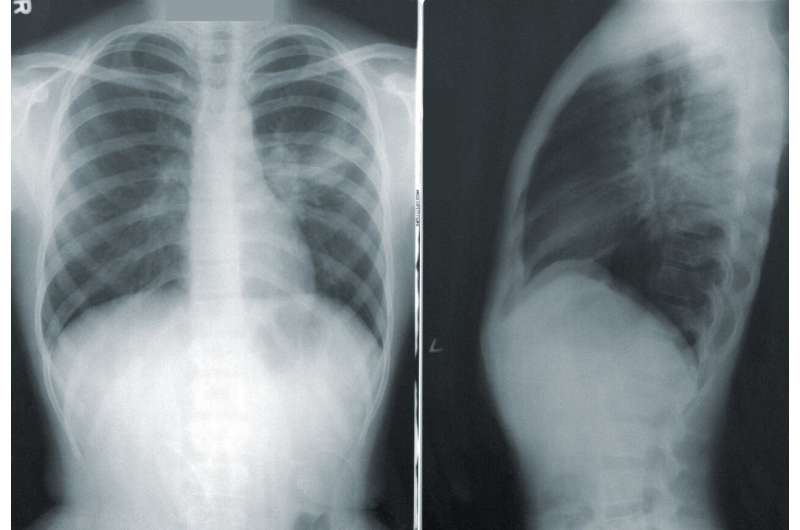
A Rutgers researcher leading a trial found that the novel combination antibiotic sulbactam-durlobactam combats dangerous pneumonia at least as well as the best currently approved treatment.
The findings have led a unanimous expert committee to recommend that the Food and Drug Administration (FDA) approve the new drug, which could be available this summer to combat the often-fatal pneumonia strain known as carbapenem-resistant Acinetobacter baumannii–calcoaceticus complex (ABC), typically acquired in hospitals.
“Antibiotic-resistant infections are a serious and persistent problem at healthcare facilities, and the [Centers for Disease Control] ranks ABC at the highest level on its threat list,” said Keith Kaye, chief of the Division of Allergy, Immunology and Infectious Disease at Robert Wood Johnson Medical School and first author of the trial report in The Lancet Infectious Diseases. “An estimated 8,500 hospital-acquired cases killed 700 patients and cost $280 million in 2019, so we greatly needed a breakthrough treatment like sulbactam-durlobactam.”
The trial gave imipenem–cilastatin to 181 patients with laboratory-confirmed ABC and then randomized them to additional treatment with either sulbactam–durlobactam or the best existing treatment, an antibiotic called colistin. Mortality due to multiple causes after 28 days was 12 of 63 (19 percent) in the sulbactam–durlobactam group and 20 of 62 (32 percent) in the colistin group.
The trial was large enough to prove that sulbactam-durlobactam prevents at least as many fatalities as colistin but not large enough to prove its superiority in this trial will persist in real-world use, though it may.
The trial results did prove that sulbactam-durlobactam beats colistin in one crucial respect: tolerability. Kidney injury, serious adverse events and all treatment-related adverse events were significantly lower for patients who received sulbactam-durlobactam than for patients who received colistin.
Another advantage of the novel antibiotic is dosing. All patients receive the same injectable dose of sulbactam–durlobactam. Doses of colistin in the study, on the other hand, varied with patient weight, so it’s considerably easier for providers to prescribe or administer the wrong amount.
As its name implies, sulbactam-durlobactam combines two drugs. Sulbactam has been approved for use since 1986, but durlobactam is new and has yet to win approval. That could change soon, however. The FDA’s Antimicrobial Drugs Advisory Committee reviewed advance results of the new trial, along with earlier studies, and recommended on April 17 that the FDA approve the new combination for ABC treatment.
FDA officials are free to reject such recommendations but almost always follow recommendations from advisory committees, which comprise independent experts on particular classes of disease and medication.
“If all moves quickly, infected patients could begin receiving sulbactam-durlobactam as part of normal clinical care the second half of this year,” Kaye said. “Unfortunately, sulbactam-durlobactam isn’t the sort of wide-spectrum antibiotic that could prove effective in treating a wide variety of antibiotic-resistant infections, but it’s very good at treating this particularly dangerous one, and that’s a significant win.”
More information:
Keith S Kaye et al, Efficacy and safety of sulbactam–durlobactam versus colistin for the treatment of patients with serious infections caused by Acinetobacter baumannii–calcoaceticus complex: a multicentre, randomised, active-controlled, phase 3, non-inferiority clinical trial (ATTACK), The Lancet Infectious Diseases (2023). DOI: 10.1016/S1473-3099(23)00184-6
Journal information:
Lancet Infectious Diseases
Source: Read Full Article