Cancer patients appeared to benefit from natural killer cells obtained from donors in an experimental method of treating cancer that involved an aggressive army of immune system fighters endowed with the ability to home in on malignant cells and destroy them.
The natural killer cells were pre-treated with nicotinamide, a compound widely known to most people as niacin, or vitamin B3. It’s a substance with a special affinity for natural killer cells, enhancing their capacity to annihilate cancers. Once primed in the laboratory, these natural killers are ready to be unleashed against formidable targets. The evolving methodology has shown promise in a preliminary study aimed at forcing hard-to-treat cancers of the blood into remission.
Prior to the new research, which is published in Science Translational Medicine, attempts by other teams to use natural killer cell infusions as a therapeutic for leukemias, lymphomas and other blood malignancies, weren’t always effective. Doctors were confronted with a problem: some people simply didn’t respond to the investigational treatment, which was offered after standard therapy failed.
Now, in a unique take on this emerging form of cancer treatment, medical scientists in the Division of Hematology, Oncology and Transplantation at the University of Minnesota, have devised a way to boost the effectiveness of natural killer cells, enhancing their role as a therapeutic. The innovative approach boosted the impact of natural killer cells and brought about remissions in patients with otherwise recalcitrant cancers.
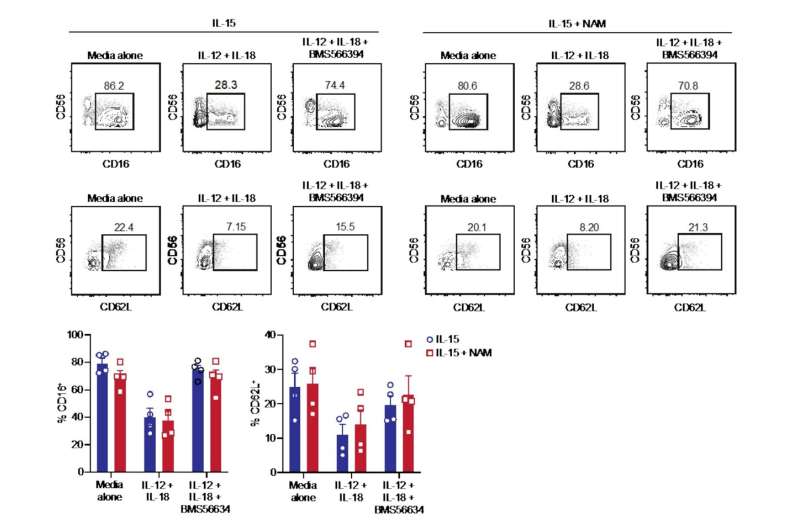
“Allogeneic natural killer cell adoptive transfer has shown the potential to induce remissions in relapsed or refractory leukemias and lymphomas,” writes Dr. Frank Cichocki and colleagues in the journal. “Strategies to enhance natural killer cell survival and function are needed to improve clinical efficacy. We demonstrated that natural killer cells cultured ex vivo with interleukin-15—IL-15—and nicotinamide exhibited stable induction of l-selectin, a lymphocyte adhesion molecule important for lymph node homing.”
Nicotimamide helps the body turn food into energy and is chemically part of the coenzymes NAD+ and NADH, which are critical in oxidation-reduction reactions throughout the body. Among these activities is the production of adenosine triphosphate, ATP, which fuels cellular and metabolic processes.
In 1937, researchers discovered that the systemic disease known as pellegra is caused by a niacin deficiency. The disorder is typified by the three D’s—dementia, diarrhea and dermatitis. Without treatment, which is simply providing niacin, pellegra can be fatal.
The team’s choice of nicotinamide as an enhancer of natural killer cells shines a spotlight on the common water-soluble compound and demonstrates how it can boost the anti-cancer activity of natural killer cells. These cells are lymphocytes and members of the innate immune system, the body’s first response to invasive disease. Natural killer cells’ job is helping control cancer and invasive microbes.
Scientists, meanwhile, who are developing the experimental therapy have merely boosted these cells to help them attack cancers more efficiently. If further testing proves this method effective—and the Minneapolis-based scientists are convinced they’re on the right track—then an innovative new approach to treating cancers of the blood will emerge.
“We conducted a first-in-human phase 1 clinical trial testing adoptive transfer of natural killer cells expanded ex vivo with IL-15 and nicotinamide combined with monoclonal antibodies in patients with relapsed or refractory non-Hodgkin lymphoma and multiple myeloma,” Cichocki asserted in Science Translational Medicine.
In the small preliminary study, Cichocki and collaborators found that nicotinamide not only enhances the activity of natural killer cells but boosts their persistence in the blood and bolsters the capability of these cells not only to hunt down cancer cells, but to handily destroy them.
The combination of nicotinamide-enhanced natural killer cells and monoclonal antibody treatment was safe in 30 patients, including 20 with relapsed or difficult-to-treat non-Hodgkin lymphoma. Among 19 patients with non-Hodgkin lymphoma, 11 demonstrated a complete response and three had a partial response within 28 days of treatment. Nicotinamide appears to protect the natural killer cells from oxidative stress, while enhancing their ability to home in on lymph nodes, the team found.
“High frequencies of CD62L were associated with elevated transcription factor forkhead box O1, or FOXO1,” Cichocki noted, referring to the homing molecule, CD62L, which shepherds natural killer cells to the lymph nodes. As a transcription factor, FOXO1 is responsible regulating a broad number of genes involved in metabolism, cell cycle progression and programmed cell death.
In cancers, FOXO1 acts as a suppressor of malignant cells mainly because of its roles promoting programmed cell death—apoptosis—and inhibiting cell cycle progression, angiogenesis and metastasis.
“Nicotinamide promoted the stability of FOXO1 by preventing proteasomal degradation,” Cichocki lead author of the study added. “Natural killer cells cultured with nicotinamide exhibited metabolic changes associated with elevated glucose flux and protection against oxidative stress.”
Natural killer cells treated with nicotinamide in the lab also demonstrated an increased ability to generate an inflammatory and toxic response against cancer cells. Cichocki and colleagues concluded that their findings suggest the new transfer strategy should be studied further in larger clinical trials.
More information:
Frank Cichocki et al, Nicotinamide enhances natural killer cell function and yields remissions in patients with non-Hodgkin lymphoma, Science Translational Medicine (2023). DOI: 10.1126/scitranslmed.ade3341
Journal information:
Science Translational Medicine
Source: Read Full Article