Weight loss of at least 15% of body weight should become the “initial principal treatment goal” for many patients with type 2 diabetes, according to a new review and proposal published by an international quartet of diabetologists.
Although this proposition currently has formal backing from just the four authors of the article published in the Lancet, their recommendation to elevate substantial weight loss to the front line of management for many patients with type 2 diabetes drew quick support from leaders of several diabetes organizations, albeit with some caveats.
“Our main message is that treatment of obesity should be the future of diabetes treatment,” summed up Ildiko Lingvay, MD, lead author of the new review and proposal, at the annual meeting of the European Association for the Study of Diabetes.
“Right now, a relatively small percentage of clinicians [who treat patients with type 2 diabetes] address obesity and know how to treat it. That has to change. Every clinician who treats diabetes needs to know how to treat obesity,” said Lingvay, a professor in the division of endocrinology at the University of Texas Southwestern Medical Center, Dallas.
This requires a sea change in the way clinicians approach treating patients with type 2 diabetes, which until now has generally involved “exclusive focus on glycemic control,” the authors wrote. “Practice management should refocus to effectively incorporate weight management to treat patients with type 2 diabetes.”
Successfully implementing their new, proposed change in focus “will take fundamental change,” noted Lingvay, who expressed hope that international guidelines will soon endorse this approach, an action that would be “a huge step in the right direction.”
Target Weight-Loss Drugs to the Right Patients
Initial reactions from representatives of several diabetes and obesity groups suggested that official endorsements of this management strategy for at least a subset of patients with type 2 diabetes may be forthcoming.
“The American Diabetes Association’s standards of care is aligned with this approach in focusing on obesity as a target of management in people with type 2 diabetes,” commented Nuha A. El Sayed, MD, vice president for health care improvement for the ADA. An “area of discussion” is the specific weight-loss target of at least 15%, because patients benefit from more modest weight losses of 5%-7%, and a target loss of 15% may not be achievable for some patients, she noted in a statement.
The ADA’s leadership and its professional practice committee will “carefully consider” the new, published proposal, added El Sayed, a diabetologist at the Joslin Diabetes Center in Boston.
Similar caution over generalizability of the 15% loss target came from Stefano Del Prato, MD, president of the European Society for the Study of Diabetes.
“Not everyone responds to the same extent” to the newest pharmaceuticals for facilitating weight loss, such as the glucagonlike peptide-1 receptor agonists, so the ideal would be to try to “identify patients who respond better to weight loss and can lose at least 15% of their weight. We need to improve our ability to identify patients who respond better,” said Del Prato, a professor of endocrinology and metabolism at the University of Pisa (Italy).
Despite this, he agreed in an interview that “a significant reduction in body weight should be seen as a target for treatment of type 2 diabetes,”
“Appropriate training for obesity management is essential for those working on type 2 diabetes prevention or management,” commented Jason C.G. Halford, PhD, a professor of biological psychology at the University Of Leeds (England), and president of the European Association for the Study of Obesity.
For some patients with type 2 diabetes “losing 10%-15% of body weight can mean their diabetes goes into remission,” and “losing even a small amount of weight can be life changing, it can help people better manage their blood sugars and blood pressure, and reduce their risk for developing diabetes complications like heart disease and sight loss,” commented Lucy Chambers, PhD, head of research communications for Diabetes UK.
15% Loss Is a “Reachable” Goal
Lingvay and coauthors acknowledged that weight loss of less than 15% can benefit many patients with type 2 diabetes, but they felt that a loss of at least 15% gives patients a realistic and potentially potent goal to strive for.
At least 15% loss “is a goal that is beneficial and reachable for many patients. Not everyone will get there, but the closer that patients get to this, or beyond, the bigger their benefit,” she explained. “There is no magic number” for exactly how much weight a patient needs to lose to improve their health. Lingvay also highlighted that weight loss is a better target for patients than remission of their diabetes because remission may no longer be possible in patients with longstanding type 2 diabetes.
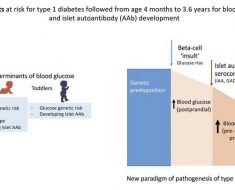
The review divides patients with type 2 diabetes into three subgroups: those with adiposity-related disease, which includes about 40%-70% of patients with type 2 diabetes; patients with cardiovascular disease as their most prominent comorbidity, a subgroup that includes about a third of patients with type 2 diabetes; and the remaining patients with primarily beta-cell dysfunction with a principle morbidity of hyperglycemia, comprising about 10%-20% of patients with type 2 diabetes. Patients in the adiposity-related diabetes subgroup form the primary target group for interventions focused on weight loss.
Incretin-Based Weight-Loss Agents Propel Change
The review also links the timing of the new recommendations to recent evidence that treatment with relatively new medications from classes such as the GLP-1 receptor agonists can produce weight loss of at least 15% in most patients with type 2 diabetes, especially those with the adiposity-related form of the disease.
“The number of patients who can achieve and maintain weight loss with lifestyle alone is limited, and while bariatric surgery is very effective [for producing substantial weight loss], only a minority of patients have access to it,” and the necessary scalability of surgery is doubtful, said Priya Sumithran, MBBS, PhD, an endocrinologist and leader of the obesity research group at the University of Melbourne, and a coauthor on the new review. Compelling evidence now exists that the gap between lifestyle interventions and bariatric surgery can now be filled by a new generation of incretin-based agents that can safely produce substantial weight loss.
New agents that work as GLP-1 receptor agonists and on related incretin pathways “have changed how we think about treating type 2 diabetes,” Lingvay declared.
Lingvay and Del Prato have each been consultants to numerous drug companies. Sumithran has been an adviser to and speaker on behalf of Novo Nordisk. El Sayed, Halford, and Chambers had no relevant disclosures.
This article originally appeared on MDedge.com, part of the Medscape Professional Network.
Source: Read Full Article