A Finnish study published in the respected SLEEP journal shows that a variation in the melatonin receptor 1A (MTNR1A) gene is linked to the risk of Alzheimer’s disease in the elderly. The same research team has previously demonstrated that the same genetic variation reduces tolerance to shift work among the working age population.
Alzheimer’s disease is a memory disorder that causes the brain to deteriorate. One of its risk factors is disruption of sleep and the circadian rhythm. Lack of sleep and disruption of the circadian rhythm are common among shift workers. Tolerance to the negative effects of shift work varies between individuals and is partially linked to intrinsic genetic factors.
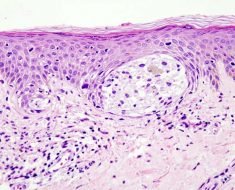
The study lead by Professor Tiina Paunio, University of Helsinki and National Institute for Health and Welfare (THL), Finland, showed that in addition to Alzheimer’s diagnosis, the MTNR1A gene variation is linked to brain lesions visible in post-mortem brain tissues. In addition, when the expression of the MTNR1A gene was reduced in the cell culture, beta-amyloid protein characteristic of Alzheimer’s disease started to accumulate.
The previous study observed that the same gene variation that predisposes to shift work fatigue is associated with lower levels of the MTNR1A gene expression in the brain. This means that the previous findings are compatible with the new findings made in the epidemiological cohorts and cell cultures.
A genetic predisposition combined with a lifestyle that disrupts the circadian rhythm can increase the risk of Alzheimer’s disease
The circadian rhythm regulates the release of melatonin, which in turn supports the circadian rhythm through its receptors. The link between a weaker signalling of endogenous melatonin and Alzheimer’s disease supports the view that regulation of the circadian rhythm plays a role in the development of Alzheimer’s disease.
“The finding of a common risk gene for both job-related exhaustion in shift workers and Alzheimer’s disease doesn’t directly mean that shift work would predispose to Alzheimer’s disease. However, the combination of genetic predisposition and a lifestyle that disrupts the circadian rhythm can increase the risk of Alzheimer’s disease,” says Lic. Med Sonja Sulkava from the National Institute for Health and Welfare (THL). “Another possible interpretation is that the brain dysfunctions related to Alzheimer’s disease impair the tolerance to shift work decades before the onset of the clinical disease.”
“Even though our results demonstrate a new molecule-level connection between the tolerance to shift work and incipient Alzheimer’s disease, the now discovered genetic variation has a minimal effect on the individual level and it can’t be used to risk assessment or prediction,” reminds professor Paunio.
Source: Read Full Article