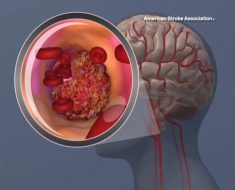
Each year, roughly 15,000 Americans are diagnosed with Glioblastoma Multiforme (GBM), the most common malignant primary brain tumor in adults, and also the most lethal. Surgery, radiation, and chemotherapy can help slow the tumor’s growth, but the disease remains incurable. Recurrence occurs in almost every case.
While the median survival rate is counted in months, there are survivors who have lived in remission for years, some for more than a decade.
While all treatments help improve outcomes, immunotherapy is potentially a “game changer,” says Donald O’Rourke, director of the GBM Translational Center of Excellence at the Abramson Cancer Center.
“We need an approach that goes places where surgeons can’t … the deeply invasive portions of the tumor,” he continues. “We need to harness and engineer the patient’s immune system.”
The Challenges of Curing GBM
For a number of reasons, glioblastomas are in a class of their own, said Stephen Bagley, MD, of Hematology/Oncology, making them “extremely difficult to treat.”
Their location is part of the problem. A natural blood-brain barrier prevents poisons and toxins from getting into the brain. As a result, “all the chemo drugs and targeted therapies revolutionizing other cancers simply don’t penetrate, so they’re not even accessing the tumor.”
Also, by the time GBM is first diagnosed, it is usually widespread in the brain. “While you might only see one mass on an MRI scan and during surgery, microscopic cancer cells are infiltrating other parts, using nerve tracks in the brain as a highway,” Bagley said.
GBM is heterogeneous, meaning not all of its cells are the same. “With certain types of lung cancer, all of the cancer cells have a similar genetic makeup, no matter where they are in the body,” he explained. “This means if we can target a particular protein on the lung cancer cell with a drug, we’re getting the vast majority of them.” However, two GBM cells, located right next to each other, can have a totally different molecular makeup. “That’s heterogeneity… and it’s a major problem.”
In addition, the GBM tumor has many ways of making itself invisible to the immune system. “If you slice open a lung cancer or melanoma tumor and look at it under the microscope, you’ll see T cells [the body’s ‘killer cells’] trying to fight the tumor,” Bagley said. “With GBM, there are very few T cells trying to get in. They don’t recognize the tumor as foreign.”
The tumor’s ecosystem also presents a challenge. The body’s immune system has safety checkpoints which prevent T cells from destroying healthy cells. However, cancer cells can co-opt these checkpoints to turn the T cells off, thus preventing them from destroying the cancer cells.
Still, although the challenges remain great, the mechanisms behind them are becoming much better understood. “We are tackling each problem individually,” Bagley said. “They’re small steps … but taken together, we are getting somewhere.”
Overcoming the Barriers
Chemotherapy, radiation, and surgery help to reduce the volume of a tumor to a minimal residual disease, enabling a patient’s own immune system to fight back. Advances in “seeing” the tumor enable surgeons to remove more of it with minimal impact to brain function. For example, an injectable fluorescent material taken up by cancer cells renders them visible using a special infrared camera. Advanced diffusion tractography—a brain mapping technology—helps the neurosurgeon avoid key tracts.
“If you can tell the wiring of the brain, you can remove a lot of the tumor and still keep the patient whole,” said Steven Brem, MD, director of Neurosurgical Oncology. And radiation therapy is better able to zero in on the tumor as well, “keeping a patient’s cognitive ability, which used to be a big problem.”
Recurrence occurs in almost every patient, but a phase II clinical trial at Penn is investigating a mathematical model that can predict where a tumor might recur based on pre-operative MRIs. “If we can analytically select where tumors are most likely to recur and treat those areas to high dose radiation, we can decrease the doses to normal tissue, lowering the risk of complication and increasing our local control of the tumor,” said Robert Lustig, MD, of Radiation Oncology.
Multidisciplinary researchers at the TCE are investigating several immunotherapy strategies that target both the tumor and the tumor’s microenvironment. “We’re seeking ways to stop the resistance of—or increase the persistence of—functional T cells,” O’Rourke said.
One is the use of CAR (chimeric antigen receptor) T cells, a personalized cellular therapy that uses engineered versions of a patient’s T cells to target specific antigens on the cancer cell. O’Rourke explained that, once infused back into the patient’s body, these cells create a “living drug” that stays in the body and remodels the immune system. A phase l trial now underway targets the GBM antigen known as EGFRvIII (epidermal growth factor receptor, variant III), in patients with newly diagnosed disease. “This is the first trial to do this in a solid tumor,” O’Rourke said. “The hope is that killing some of the tumor cells will cause them to die and release their contents into the brain and blood and this, in turn, will bring in other immune cells to attack them.”
It’s cutting edge, but more trials are needed, focusing on different antigens. “If we can target maybe four antigens that are each present in 30 to 50 percent of patients, together they cover everyone statistically,” Bagley said. “We want to cast a wider net.”
Researchers are also combining potential treatments with checkpoint inhibitors (CPIs)— drugs that target the immune checkpoints—which then “take the brakes off the controls in the immune system, enhancing the immunological response to a particular target,” O’Rourke said. An upcoming investigation will combine two CPI drugs with stereotactic radiosurgery in patients with recurrent GBM. This type of radiation therapy delivers precisely-targeted radiation in fewer, high-dose treatments than traditional therapy, which can help preserve healthy tissue. Other trials are investigating injecting certain viruses directly into the tumor, infecting cancer cells. Similar to CAR T cells, they cause a tumor to break open and release its antigens, signaling the immune system to attack.
In addition, in a new study, Penn researchers were the first to show that a liquid biopsy—a blood test that measures the amount of cell-free DNA (cfDNA) in the bloodstream—correlates with how patients will progress after they are diagnosed with GBM. Those with more cfDNA will have a shorter progression-free survival than patients with less cfDNA. Researchers also found that they could learn more about the molecular or genetic makeup of each tumor from the liquid biopsy.
“If our findings are validated by further studies, it would mean that these patients may be able to get a simple blood test that would give us a more accurate assessment than imaging of whether their disease has progressed or not, as well as more data on the mutations in their tumors,” said Bagley, who is the study’s lead author. Findings were published in Clinical Cancer Research, a journal of the American Association for Cancer Research.
O’Rourke sees potential in giving multiple infusions of engineered T cells to increase their persistence in targeting tumor cells, and, down the road, having having ready-made engineered T cells that are predesigned to meet certain patients’ needs … and immediately available. He also hopes to speed up the process of transitioning pre-clinical models of immune system treatments into clinical trials, allowing them to get these new, potentially life-saving treatments to patients more quickly.
Source: Read Full Article